Transoral robotic surgery (TORS) has emerged as a revolutionary option in the field of surgical oncology, offering patients a minimally invasive technique to address various tumors and conditions of the head and neck. This advancement represents a paradigm shift from traditional surgical methods and holds promise for not only improving surgical outcomes but also enhancing recovery experiences for patients.
A Brief Insight into TORS
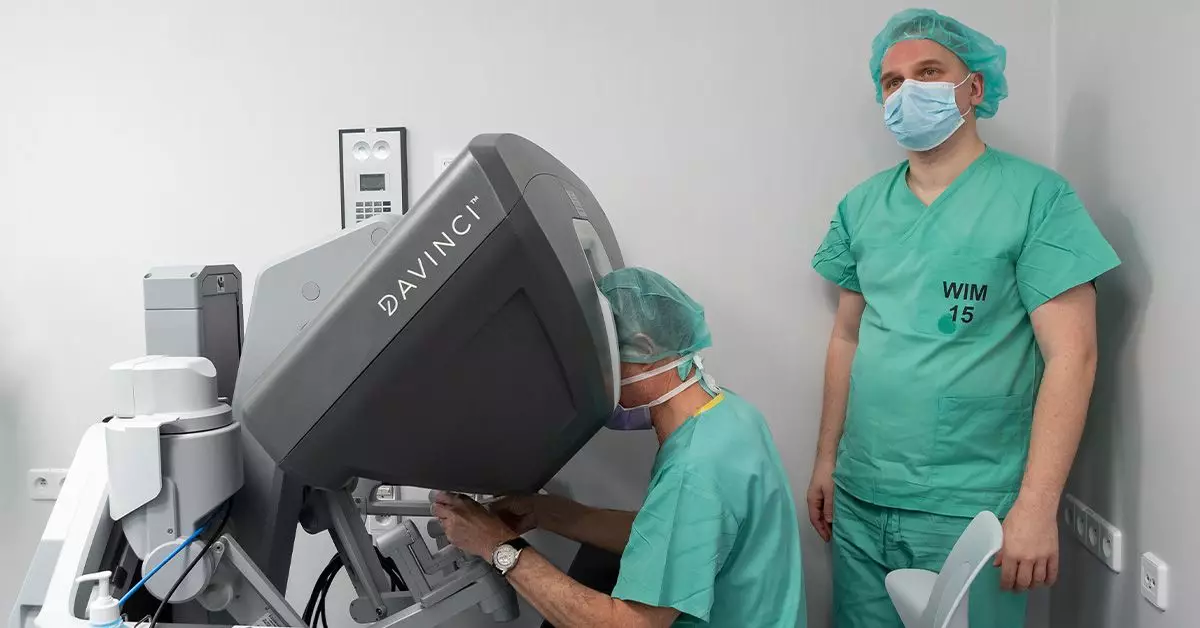
At the heart of TORS is the Da Vinci Robotic System (DVRS), a state-of-the-art technology that allows surgeons to perform delicate procedures through the oral cavity—a significant advantage compared to conventional techniques that require external incisions. The DVRS utilizes three sophisticated articulated arms that replicate a surgeon’s hand movements with precision. The central arm is equipped with a high-definition camera, while the secondary arms serve as the functional hands of the robotic system. This setup permits surgeons to navigate the challenging anatomical landscape of the head and neck with great dexterity.
The allure of TORS lies in its minimally invasive nature, which can lead to various patient benefits, including reduced surgical trauma and expedited recovery. The FDA approved TORS for specific uses in 2009, primarily targeting benign tumors and early-stage cancers, thus marking a noteworthy milestone in surgical options for head and neck conditions.
Clinical Benefits and Comparisons
Recent studies have begun to unravel the various advantages associated with TORS compared to traditional surgical approaches. A comprehensive review published in 2022 examined a large cohort of patients suffering from oropharyngeal cancer, comparing TORS with nonrobotic surgery (NRS) and nonsurgical treatment (NST). The findings consistently highlighted that TORS maintained exceptional safety profiles and markedly lower rates of severe complications relative to NRS. Notably, TORS showed a higher success rate in completely excising cancerous cells, with the efficacy improving as surgical teams gained experience with the robotic system.
Interestingly, hospitals performing TORS frequently—at least 10 procedures annually—demonstrated notably better patient outcomes, underscoring the importance of experience and specialization in enhancing surgical success rates.
Feasibility and Safety of TORS
A small-scale study published in 2023 further corroborated TORS’s feasibility as both a diagnostic and therapeutic modality for squamous cell carcinoma (SCC) of the head and neck. The results underscored TORS’s capability in accurately detecting primary tumors, a crucial step in developing effective treatment strategies for cancer patients. The minimally invasive approach of TORS offers a plethora of benefits, including shorter hospital stays and reduced recovery times, which are significant considerations for patient quality of life post-surgery.
Despite its advantages, it’s pertinent to note that TORS is not devoid of risks. Like any surgical procedure, TORS carries certain risks, including potential human error and mechanical failures. However, the incidence of such complications remains exceedingly low, estimated at around 0.1% to 0.5%.
Following TORS, patients may initially find swallowing challenging, necessitating a temporary feeding tube for nutritional intake. Recovery trajectories vary widely based on individuals’ overall health and the surgery’s extent. While many patients may return to liquids shortly after surgery, transitioning to soft foods typically occurs within a few days. Healthcare teams remain actively involved in monitoring and facilitating recovery, often incorporating specialists to aid in swallowing rehabilitation.
Hospital stays generally range from three to ten days, with most individuals requiring at least six weeks away from work to ensure full recovery. Regular follow-up appointments become essential, particularly for patients with head and neck cancer, as these visits focus on monitoring for cancer recurrence and assessing ongoing needs for adjunctive treatments like chemotherapy or radiation.
Robotic surgery not only benefits patients but also bolsters the surgeons’ experience by reducing physical stress and mental fatigue associated with prolonged procedures. The increased dexterity afforded by robotic assistance translates to enhanced precision during sensitive operations, allowing surgeons to focus on overall patient care rather than the physical demands of traditional surgery.
A notable theme emerging from the literature is the promising efficacy of TORS in ensuring faster healing and a smooth postoperative journey, contributing to a more favorable outlook for patients undergoing head and neck interventions.
Transoral robotic surgery is becoming an increasingly integral element of the surgical treatment landscape for various head and neck conditions. As research continues to validate its safety and effectiveness, TORS represents an attractive alternative to conventional surgical techniques. Prospective patients should actively engage in discussions with their healthcare providers to ascertain if TORS may be a fitting option based on their unique clinical circumstances. Overall, the advancements in robotic surgery herald a new era in surgical oncology, promoting both improved patient outcomes and enhanced surgical precision.